PEACE Project
What is the PEACE Project?
Under the Cancer Control Act of 2006, the government has developed a comprehensive cancer strategy, which aims, among other things, to promote basic awareness about palliative care among physicians involved in cancer care. To this end, the strategy provided a set of guidelines for running palliative training programs for such physicians (Guidelines for Organizing Palliative Care Training Programs for Physicians who Engage in Cancer Care).
Commissioned by the Ministry of Health, Labour and Welfare, the Japanese Society for Palliative Medicine worked with the Japan Psycho-Oncology Society to develop an educational program based on the training guidelines. The program is titled PEACE (Palliative care program Emphasizing symptom management and Assessment for Continuous medical Education).
The objective of PEACE is to equip physicians with the basic knowledge, skills, and attitudes concerning palliative care. To accomplish this objective, we designed the learning content with a focus on four palliative care-related competences for post graduate 3 physicians. The four competences are: 1. the basic sensitivity to realize pain (suffering) sustained by a patient or family member and to ask them about it; 2. the basic palliative care skill to address, in addition to cancer-related pain, physical symptoms (other than physical pain), emotional pain, delirium, and other psychological symptoms; 3. basic communication skills; 4. the knowledge about services provided by local organizations and the home healthcare system with a view to helping the patient stay in the desired environment
Initially, the program ran for two days and consisted of lectures and a workshop. The workshop involved roleplaying and case studies.
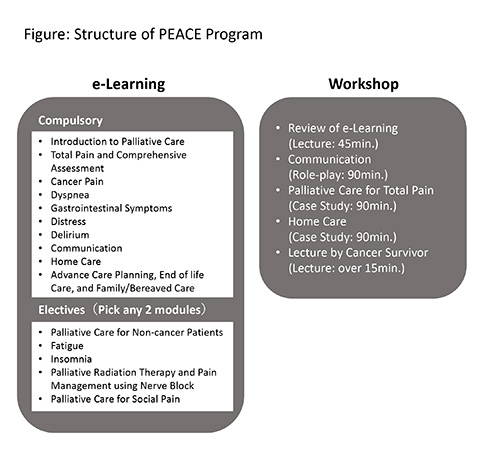
In 2017, the government released its third comprehensive cancer strategy, which led to a revised version of the training guidelines (Guidelines for Organizing Palliative Care Training Programs for Physicians and other Practitioners who Engage in Cancer Care and Other Care). The revised guidelines provided that the programs should offer e-learning in combination with a one-day group workshop. Figure shows the current learning content. Please visit the PEACE e-Learning website for more information (https://peace.study.jp/pcontents/top/1/index.html; in Japanese only).
The program offers various benefits. Those who complete the program will have systematically mastered the basic knowledge on palliative care, and they will also be able to earn extra fees for instructing and managing cancer-related palliative care.
The Educational Outcomes of PEACE
Although it is difficult to measure the program’s direct effects, a number of studies have demonstrated that the program is effective. First, Yamamoto et al. (2013)1 developed a scale to measure palliative care knowledge, and used it to determine the program’s outcomes. Using this scale, the authors conducted a questionnaire survey among the program attendees before, soon after, and two months after the program, to measure changes in the participants’ knowledge and subjective difficulties concerning palliative care. The results indicated that knowledge was significantly higher soon after the program and that it remained high two months later. This finding was supported by Yamamoto et al. (2015),2 who reported that subjective difficulties were significantly reduced after program completion. This indicated that the program has an effect to a certain extent. Additionally, Nakazawa et al. (2018)3 analyzed two large-scale studies from 2008 and 2015, which measured the knowledge and subjective difficulties of program attendees. The analysis revealed that the physicians’ knowledge and subjective difficulties had significantly improved. The same study also conducted propensity score matching, which indicated that physicians who attended the program had better knowledge and lower subjective difficulties than those who did not.
References
- Yamamoto R, et al: The Palliative care knowledge questionnaire for PEACE: reliability and validity of an instrument to measure palliative care knowledge among physicians. J Palliat Med 16(11): 1423-8, 2013
- Yamamoto R, et al: Outcome evaluation of the palliative care emphasis program on symptom management and assessment for continuous medical education: Nationwide physician education project for primary palliative care in Japan. J Palliat Med 18(1): 45-49, 2015
- Nakazawa Y, et al: Improved knowledge of and difficulties in palliative care among physicians during 2008 and 2015 in Japan: Association with a nationwide palliative care education program. Cancer 124(3): 626-35, 2018
Figure: Structure of PEACE Program